Inpatient Care for Depression 101
When Depression Becomes a Crisis: What Inpatient Care Really Means

Inpatient care for depression is a short-term, intensive treatment program where you stay at a facility 24/7 to get stabilized, safe, and back on track — typically lasting 5 to 10 days.
Here’s a quick overview of what it involves:
- Who it’s for: Adults with severe depression who are unsafe, unable to function, or not improving with outpatient treatment
- What happens: Round-the-clock supervision, medication management, individual and group therapy, and crisis stabilization
- How long it lasts: Usually 5 to 10 days on average, depending on your symptoms and progress
- What comes next: A step-down plan to Partial Hospitalization (PHP) or Intensive Outpatient (IOP) for continued recovery
- Cost: Often covered by Medicare or private insurance, though costs vary by plan
Depression is one of the most common mental health conditions in the United States. An estimated 21 million adults experienced at least one major depressive episode in 2020 alone. For most people, outpatient therapy and medication are enough. But for some, depression becomes so severe that daily life — eating, sleeping, working, staying safe — falls apart.
That’s when inpatient care becomes not just helpful, but necessary.
If you’re in New Jersey and wondering whether you or someone you love has reached that point, this guide walks you through everything you need to know — from what happens on day one to what recovery looks like long-term.
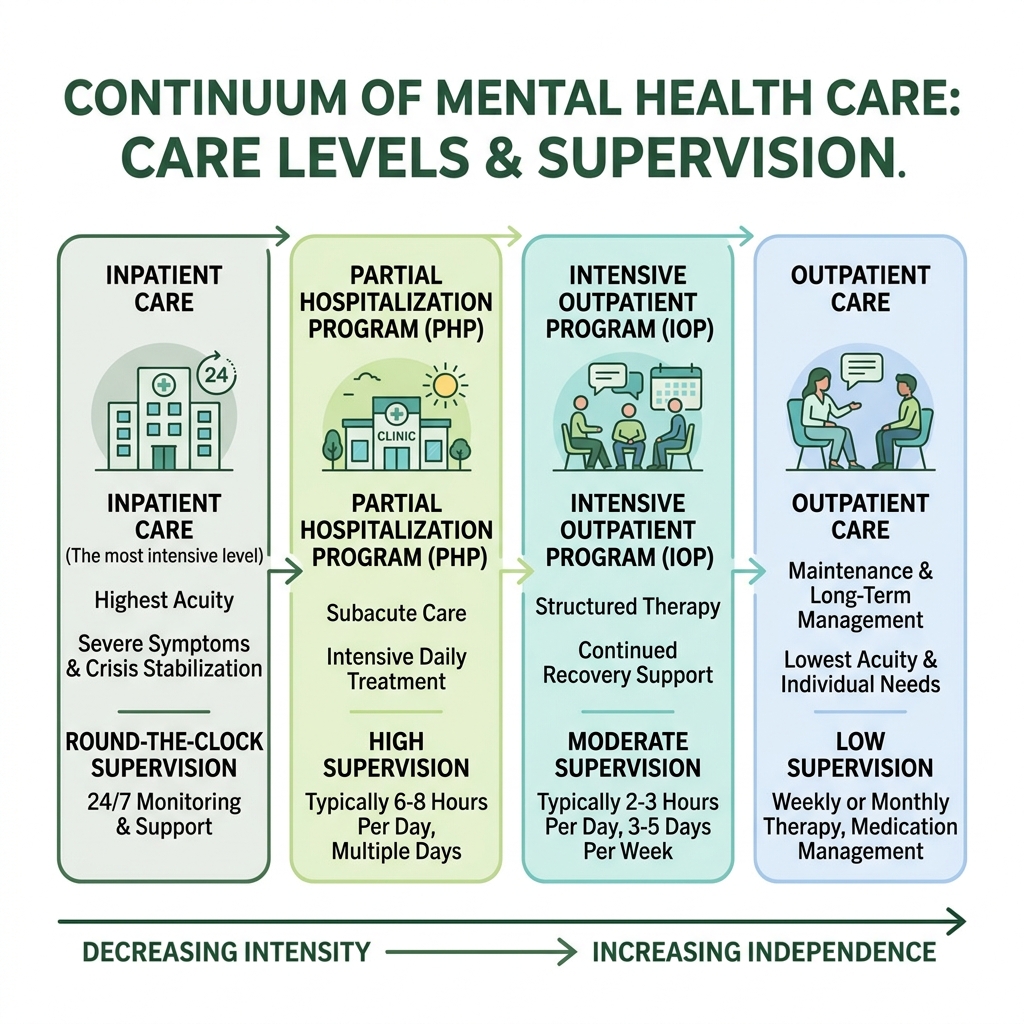
Understanding Inpatient Care for Depression
When we talk about inpatient care for depression, we aren’t talking about a “forever” solution or a place where people are “sent away.” Modern inpatient care is a high-intensity clinical environment designed for one thing: stabilization.
According to the 2020 National Survey on Drug Use and Health, depression affects people of all ages and walks of life. While many manage their symptoms through weekly therapy, about 18.3 percent of U.S. adults are currently experiencing depression, and for a portion of them, the symptoms become life-threatening or debilitating.
Inpatient care differs from residential treatment. While residential programs might last 30, 60, or 90 days in a home-like setting, inpatient care usually happens in a hospital or specialized psychiatric facility. The focus is on safety monitoring and acute stabilization. Think of it as the “ER for the soul.” If you were having a heart attack, you’d go to the hospital to get stabilized before going to cardiac rehab. Inpatient care is the mental health equivalent for a severe depressive crisis.
We often see patients who feel like they’ve failed because they need this level of care. We want to be clear: needing a higher level of support is a clinical reality, not a personal failure. In a safe, structured environment, you are removed from the stressors of daily life—the bills, the difficult relationships, the work pressure—so you can focus entirely on your brain health. For more context on how these services fit into the local landscape, check out this More info about depression treatment in New Jersey.
Identifying the Need for Intensive Stabilization
How do you know when “feeling down” has crossed the line into needing 24/7 care? It usually comes down to safety and functionality. If depression has made it impossible to meet your basic needs—like eating, bathing, or getting out of bed for days at a time—that is a sign of severe functional impairment.
Another major indicator is “treatment failure.” This happens when someone has tried several medications, attended weekly therapy, and perhaps even tried an intensive outpatient program, but their symptoms continue to worsen. When depression doesn’t respond to standard care, we call it treatment-resistant depression. You can learn more about the signs of treatment-resistant depression and why a hospital setting might be the best place to recalibrate your treatment plan.
In some cases, depression can even include psychotic symptoms, such as hallucinations or delusions, or a level of persistent hopelessness that makes it impossible to see a future. These are red flags that require immediate, professional intervention in a controlled setting.
When is Inpatient Care for Depression Necessary?
The most critical reason for inpatient care for depression is immediate safety. This includes:
- Suicidal Ideation: If you or a loved one are having thoughts of ending your life, especially if there is a plan or intent to act on those thoughts.
- Self-Harm Risk: Engaging in behaviors that cause physical harm to yourself.
- Active Intent: A clear and present danger to yourself or others.
- Medication Crisis: If a medication change has caused a severe adverse reaction or a sudden spike in suicidal thoughts.
If you are in an immediate crisis, The Suicide & Crisis Lifeline is available 24/7 by calling or texting 988.
Inpatient care provides a “safety net.” In a facility, you are under constant supervision, which prevents self-harm while doctors work to find the right combination of therapies to lift the fog of depression. It is the fastest way to ensure someone stays alive long enough for the treatment to start working.
The Therapeutic Process and Daily Routine

Once you are admitted, the process begins with a thorough assessment. We don’t just look at your mood; we look at your medical history, your physical health, your family dynamics, and any co-occurring issues like anxiety or substance use.
In an inpatient setting, you aren’t just seeing one doctor. You are supported by a multidisciplinary team that typically includes:
- Psychiatrists: To manage and adjust medications.
- Nurses: To monitor your physical health and safety 24/7.
- Social Workers/Case Managers: To help with discharge planning and family communication.
- Therapists: To lead individual and group sessions.
What to Expect During Inpatient Care for Depression
A typical day in inpatient care is highly structured. Depression thrives on isolation and lack of routine; inpatient care fights back with a schedule that keeps you engaged.
While every facility is different, you can generally expect:
- Morning Check-ins: Meeting with your treatment team to discuss how you’re feeling.
- Group Therapy: This is a cornerstone of treatment. Sharing experiences with others who “get it” reduces the stigma and isolation of depression.
- Individual Counseling: One-on-one time to dive deeper into your specific triggers and goals.
- Medication Management: Doctors can monitor how you react to new medications in real-time, making adjustments much faster than they could in an outpatient setting.
- Evidence-Based Therapies: You will likely participate in Cognitive Behavioral Therapy (CBT) to challenge negative thought patterns and Dialectical Behavior Therapy (DBT) to learn emotional regulation skills.
- Advanced Treatments: For severe cases, some facilities offer Electroconvulsive Therapy (ECT). While it has a scary reputation in movies, it is actually a highly effective, modern medical procedure. For example, McLean Hospital’s ECT Service delivers over 10,000 treatments per year for depression with high success rates.
- Holistic Activities: Many programs include yoga, art therapy, or mindfulness to help connect the mind and body.
For those looking specifically at New Jersey options, here are 5 things to know about inpatient mental health in NJ.
Comparing Inpatient vs. Outpatient Treatment Models
Choosing the right level of care is about matching the “dose” of treatment to the severity of the illness. You wouldn’t use a band-aid for a broken leg, and you wouldn’t necessarily need a full cast for a small scratch.
| Feature | Inpatient Care | Partial Hospitalization (PHP) | Intensive Outpatient (IOP) |
|---|---|---|---|
| Supervision | 24/7 Medical Monitoring | Daytime (approx. 6 hours/day) | 9–15 hours per week |
| Living Situation | Stay at the facility | Go home at night | Go home at night |
| Medical Necessity | High (Crisis/Unsafe) | Moderate (Needs daily structure) | Low to Moderate (Transitioning) |
| Primary Goal | Safety & Stabilization | Skill Building & Stability | Maintenance & Reintegration |
| Duration | 5–10 days (Average) | 2–4 weeks | 8–12 weeks |
Inpatient care is the most restrictive but also the most supportive. Once you are stable, you might “step down” to a PHP or IOP. This allows you to practice the skills you learned in a real-world setting while still having a high level of professional support. If you are researching facilities in our area, take a look at the Top inpatient mental health facilities in NJ.
Financial Considerations and Insurance Coverage
We know that one of the biggest stressors when seeking help is the cost. It’s hard to focus on healing when you’re worried about the bill. However, most major insurance plans, including Medicare, provide coverage for inpatient mental health services.
Medicare Part A (Hospital Insurance) covers mental health care services when you’re admitted as an inpatient. One important detail to note: Medicare has a 190-day lifetime limit for stays in specialized psychiatric hospitals. However, if you receive care in a psychiatric unit within a general hospital, that limit may not apply.
For 2026, Medicare costs generally include:
- Days 1–60: $0 coinsurance after you pay your Part A deductible (which is $1,736).
- Days 61–90: $434 per day.
- Days 91 and beyond: $868 per day for “lifetime reserve days.”
Private insurance coverage varies wildly. Most plans require “prior authorization,” meaning the facility has to prove to the insurance company that the stay is medically necessary. Our team at True Life Care can often help navigate these conversations. For more details on navigating these systems locally, see this depression-treatment-new-jersey-guide/.
Transitioning to Long-Term Recovery and Aftercare
The day you leave the hospital is not the end of your journey—it’s the beginning of the next phase. Discharge planning starts almost as soon as you arrive. We want to make sure that when you walk out those doors, you have a “warm handoff” to your next level of care.
Research shows that having a follow-up appointment within seven days of discharge significantly reduces the risk of relapse and readmission. A successful aftercare plan usually includes:
- Step-down Programs: Transitioning to a Partial Hospitalization Program (PHP) or Intensive Outpatient Program (IOP) to maintain structure.
- Medication Continuity: Ensuring you have your prescriptions and a scheduled appointment with an outpatient psychiatrist.
- Relapse Prevention: Identifying your personal “triggers” and having a written plan for what to do if symptoms return.
- Support Systems: Connecting with local support groups or family therapy.
Family involvement is huge. Depression can be isolating for the family, too. Including your loved ones in the process helps them understand how to support you without “hovering” and helps repair relationships that may have been strained during the crisis. For a deeper dive into how we handle this transition, read our Guide to depression treatment in New Jersey.
Frequently Asked Questions about Inpatient Depression Care
How long does inpatient treatment typically last?
While it depends on the individual, the average inpatient stay for depression in the U.S. ranges from 5 to 10 days. The goal is not a “cure”—since depression is often a chronic condition—but rather stabilization. Once you are no longer in immediate danger and can follow a basic self-care routine, you are usually ready to transition to a step-down program like PHP or IOP.
Can I admit myself voluntarily to a facility?
Yes! In fact, most admissions for depression are voluntary. You can go to a local emergency room for an evaluation, or a mental health provider can refer you. Choosing to go voluntarily is a brave step toward taking control of your health. Involuntary admission only happens when a person is an imminent danger to themselves or others and refuses care.
Will my employer be notified of my treatment?
No. Your privacy is protected by federal laws, specifically HIPAA. Your employer does not have a right to your medical records or the specific reason for your absence. If you need to take time off under the Family and Medical Leave Act (FMLA), your doctor will provide documentation that you have a medical condition requiring care, but they do not have to disclose “depression” or “psychiatric hospitalization” to your boss.
Conclusion
At True Life Care, we understand that seeking inpatient care for depression is a monumental decision. It is an act of courage and a commitment to your future self. Our holistic approach ensures that you aren’t just a diagnosis—you are a person who deserves a personalized, evidence-based path to wellness.
Whether you are in Bergen County, Morris County, or anywhere across New Jersey, we are here to provide the expert psychiatric care and flexible programming you need to empower your long-term recovery. Depression may have taken a lot from you, but it doesn’t have to take your future.
If you or a loved one are ready to take the first step toward stability and hope, learn more about Inpatient Treatment at True Life Care and let us help you find your way back to a life worth living.