Dual Diagnosis Help: 3 Essential Steps to Healing
The Intertwined Challenge of Mental Health and Substance Use

Dual diagnosis help connects you with specialized treatment for both mental health conditions and substance use disorders at the same time. Here’s what you need to know:
Quick Guide to Dual Diagnosis Help:
- What it is: Treatment that addresses mental illness (like depression, anxiety, PTSD) and addiction simultaneously.
- Why it matters: Treating only one condition often leads to relapse, as both issues fuel each other.
- Where to start: Look for integrated treatment programs that offer medical care, therapy, and medication management.
- What to expect: Personalized care plans, behavioral therapies (CBT, DBT), peer support, and long-term recovery planning.
- How to find help: Contact SAMHSA’s Treatment Locator or call a specialized dual diagnosis center.
When you’re dealing with both a mental health condition and substance use, it can feel like a trap. You might use substances to cope with anxiety or depression, or your substance use may have triggered mental health symptoms. This is called a co-occurring disorder or dual diagnosis, and it’s very common.
The good news is that recovery is possible when both conditions are treated together. Addressing just one part of the puzzle rarely works because your brain, emotions, and behaviors are all connected. Effective treatment recognizes this and helps you find a path forward.
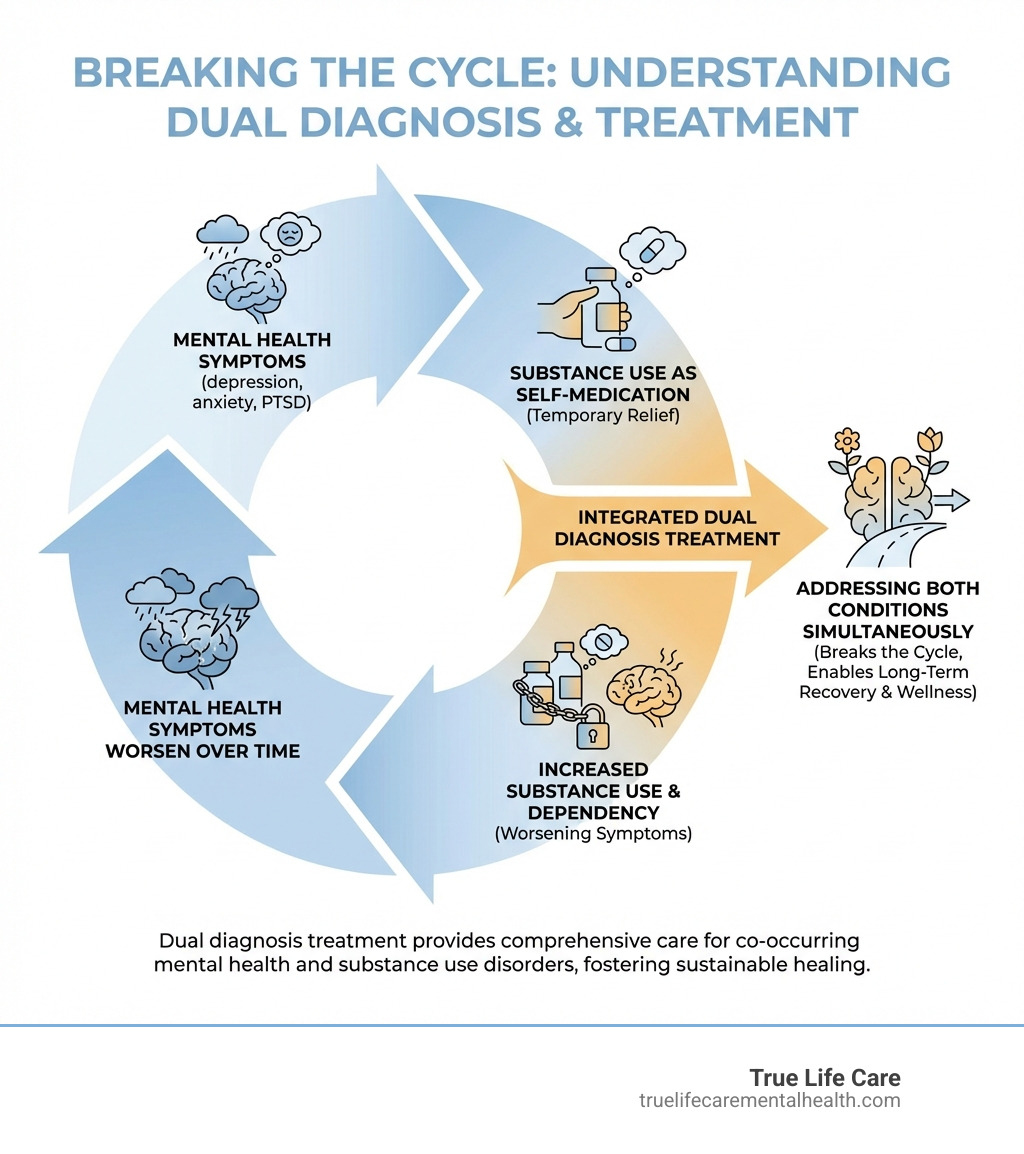
Understanding Dual Diagnosis: The What, Why, and How
A co-occurring disorder, or dual diagnosis, means an individual experiences both a mental illness and a substance use disorder (SUD) simultaneously. The conditions are intertwined; one often worsens the other. For example, someone might use substances to self-medicate mental health symptoms, or substance abuse might trigger or worsen an underlying condition. This isn’t rare; research shows a significant overlap between SUDs and mood/anxiety disorders, which is why integrated dual diagnosis help is essential for lasting recovery.
Diagnosing a dual diagnosis can be complex because symptoms often overlap. Substance withdrawal can mimic anxiety or depression, and mental health conditions can lead to behaviors that resemble addiction. A thorough, expert assessment is crucial for an accurate diagnosis and effective treatment plan.
Common Co-Occurring Conditions
Certain mental health conditions frequently co-occur with substance use disorders. Recognizing these pairings highlights the need for specialized dual diagnosis help.
- Anxiety Disorders: Individuals may use substances like alcohol or cannabis to calm nerves or escape feelings of panic and social anxiety.
- Depression: Feelings of hopelessness can lead to substance use for temporary relief, which ultimately worsens depressive symptoms.
- Bipolar Disorder: The extreme mood swings of bipolar disorder can lead to substance use to self-regulate or cope with intense emotions.
- PTSD (Post-Traumatic Stress Disorder): Many turn to substances to numb painful memories or reduce hyper-vigilance associated with trauma. The link between PTSD and SUDs is well-documented by institutions like NIDA.
- Schizophrenia: Substance use can be a way to cope with distressing symptoms, social isolation, or medication side effects.
- Personality Disorders: Conditions like borderline personality disorder often co-occur with substance use as a way to manage emotional dysregulation and impulsivity.
The National Institute on Drug Abuse (NIDA) offers extensive research on this topic, underscoring the strong link to NIDA research on comorbidity and the need for integrated treatment.
Risk Factors and Effects on Life
Several factors can increase a person’s vulnerability to developing co-occurring disorders.
Risk Factors:
- Genetic Predisposition: A family history of mental illness or addiction.
- Environmental Factors: Chronic stress from poverty, unemployment, or an unstable environment.
- Trauma: Past physical, emotional, or sexual trauma is a significant risk factor. This is why Trauma-Focused Therapy for Adults is so vital.
- Early Exposure to Substances: Using substances at a young age can disrupt brain development.
This often leads to a self-medication cycle, where substances are used for temporary relief from mental health symptoms, which in turn worsens both conditions over time. The effects of an unaddressed dual diagnosis are far-reaching, leading to strained relationships, job loss, financial hardship, severe health complications, and legal problems. Recognizing these risks underscores the urgent need for comprehensive dual diagnosis help.
Recognizing the Signs of a Co-Occurring Disorder
Identifying a dual diagnosis can be tricky, as symptoms often overlap. However, knowing what to look for is the first step toward getting the right dual diagnosis help. It’s about recognizing patterns that signal a need for professional attention.

Key indicators that might suggest a co-occurring disorder include:
- Sudden Behavioral Shifts: Becoming withdrawn, irritable, secretive, or unusually energetic.
- Difficulty Managing Daily Tasks: Neglecting responsibilities at home, work, or school.
- Social Isolation: Pulling away from friends and family in favor of being alone or with others who use substances.
- Risky Behaviors: Engaging in dangerous actions like reckless driving or unprotected sex, often while under the influence.
- Using Substances to Cope: Consistently turning to alcohol or drugs to manage stress, sadness, or other difficult emotions.
- Tolerance or Withdrawal: Needing more of a substance to get the same effect or feeling sick when trying to stop.
- Emotional Volatility: Intense mood swings, agitation, or prolonged sadness that seems disconnected from life events.
Here are more specific signs, which often appear together:
-
Mental Health Symptoms:
- Persistent sadness or hopelessness (depression).
- Excessive worry or panic attacks (anxiety).
- Flashbacks or nightmares (PTSD).
- Extreme mood swings (bipolar disorder).
- Disorganized thinking or hallucinations (schizophrenia).
- Unstable relationships and emotional dysregulation (personality disorders).
- Changes in sleep or appetite.
- Suicidal thoughts or self-harm.
-
Substance Use Symptoms:
- Inability to control or cut down on use.
- Spending excessive time obtaining, using, or recovering from substances.
- Strong cravings.
- Continued use despite negative consequences.
- Giving up important activities for substance use.
- Developing tolerance or experiencing withdrawal.
When to Seek a Professional Assessment
If you or a loved one are experiencing several of these signs, it’s time to seek professional dual diagnosis help. Early intervention can make a significant difference. Consider an assessment if you notice persistent mood or behavior changes, are unable to control substance use, or find yourself using substances to cope with emotional pain.
During a professional assessment, a clinician will conduct a comprehensive evaluation to understand your unique situation. Honesty is crucial for an accurate diagnosis and effective treatment plan. If you’re curious about the process, you can learn What to expect during an assessment. Seeking an assessment is a courageous first step toward healing.
The Path to Recovery: Finding Effective Dual Diagnosis Help
Once a dual diagnosis is identified, the next step is finding effective dual diagnosis help. The key to success is an integrated treatment approach, where both the mental health condition and the substance use disorder are treated simultaneously by the same coordinated team.
Treating both is crucial. If only the substance use is addressed, the underlying mental health issue can trigger a relapse. Conversely, treating only the mental health condition is often sabotaged by ongoing substance use. As experts like Ken Minkoff note, Best practices in integrated treatment confirm the need to address both as primary disorders.
At True Life Care Mental Health, we use a holistic care philosophy, looking at the whole person—physical, emotional, and social needs—to develop personalized treatment plans custom to your unique history and goals.
Key Components of a Dual Diagnosis Treatment Program
Effective dual diagnosis help involves a multi-faceted approach. The right level of care depends on an individual’s needs and severity of their conditions.
| Level of Care | Description | Ideal For |
|---|---|---|
| Medical Detox | Medically supervised withdrawal from substances in a safe environment to manage acute physical symptoms. | Individuals with severe physical dependence requiring medical oversight to stop use safely. |
| Inpatient Treatment | 24/7 structured care in a residential facility, providing a substance-free environment with intensive therapy and medical supervision. | Those needing constant supervision, with severe symptoms, or who need a break from their home environment to stabilize. |
| Partial Hospitalization Programs (PHP) | Intensive day treatment for several hours a day, multiple days a week, allowing individuals to return home in the evenings. | Those needing a high level of care but have a stable home environment. A step down from inpatient care. |
| Intensive Outpatient Programs (IOP) | Flexible, structured therapy for a few hours a day, several days a week, allowing individuals to maintain work or school commitments. | Individuals transitioning from higher levels of care or those needing significant support while maintaining daily responsibilities. |
| Outpatient Treatment | The least intensive care, involving weekly or bi-weekly therapy sessions to maintain recovery and build coping skills. | Individuals who have achieved stability and are focused on long-term relapse prevention. |
Comprehensive programs also incorporate behavioral therapies, medication management, case management, support groups, and life skills training.
The Role of Behavioral Therapies and Medication
We rely on evidence-based behavioral therapies and medication to address co-occurring disorders.
Behavioral Therapies:
- Cognitive Behavioral Therapy (CBT): Helps identify and change negative thought patterns and behaviors. Our Cognitive Behavioral Therapy NJ programs guide clients to challenge thinking that leads to cravings or anxiety.
- Dialectical Behavior Therapy (DBT): Teaches skills in mindfulness, distress tolerance, and emotion regulation. We offer DBT Therapy in NJ to help clients build healthier coping mechanisms.
- Motivational Interviewing (MI): A collaborative approach that strengthens a person’s own motivation for recovery.
- Trauma-Informed Therapy: Therapies like EMDR help process past trauma without relying on substances.
Medication:
Medication, monitored by our psychiatric team, can be crucial for stabilizing mental health symptoms and managing cravings.
- Medication Assisted Treatment (MAT): For opioid and alcohol use disorders, MAT combines therapy with medications to reduce cravings and prevent relapse.
- Antidepressants: SSRIs can improve mood and reduce depressive symptoms, making therapy more effective.
- Mood Stabilizers: For bipolar disorder, these medications help manage extreme mood swings.
- Anti-Anxiety Medications: May be used short-term with careful monitoring to avoid dependence.
The decision to use medication is always made in consultation with the client. Combined with therapy, it significantly improves the effectiveness of dual diagnosis help.
Navigating Long-Term Recovery and Support
Achieving initial stability with dual diagnosis help is a huge step, but recovery is a lifelong journey. Long-term success involves building a robust support system, developing healthy coping skills, and using relapse prevention strategies. It’s about empowering individuals in New Jersey and New York to live fulfilling, substance-free lives.
Key elements of long-term recovery include:
- Peer Support: Connecting with others who share similar experiences reduces isolation and provides motivation.
- Building a Sober Network: Surrounding yourself with supportive people committed to a sober lifestyle.
- Relapse Prevention: Learning to identify triggers and develop healthy responses to stress and cravings.
- Healthy Coping Mechanisms: Replacing substance use with constructive outlets like exercise, mindfulness, or hobbies. For example, good sleep hygiene is crucial for emotional regulation, as explained in The importance of sleep for mental health.
With consistent effort and the right support, the prospects for long-term recovery from a dual diagnosis are very positive.
The Power of Support Groups and Aftercare
Support groups and aftercare planning are essential for long-term dual diagnosis help. They offer ongoing encouragement, accountability, and a safe space to steer challenges.
Beneficial support groups include:
- Alcoholics Anonymous (AA) and Narcotics Anonymous (NA): 12-step programs for alcohol and drug addiction.
- Dual Recovery Anonymous (DRA): A 12-step group specifically for people with a dual diagnosis.
- SMART Recovery: A secular, self-empowering support group based on scientific methods.
Family therapy is also critical. It helps heal relationships, improve communication, and create a supportive home environment. Learning the Benefits of Family Therapy shows how it aids recovery. Continued individual and group counseling is also recommended to reinforce coping skills and address new issues.
What to Expect from Dual Diagnosis Help and Treatment
When you begin a dual diagnosis program, you can expect a structured, compassionate approach. The process starts with an initial assessment to create an individualized plan.
Throughout your program, you can expect:
- Structured daily schedules for routine and stability.
- Group and individual therapy for personal insight and peer support.
- Educational workshops on addiction, mental health, and coping skills.
- Holistic activities like mindfulness, yoga, or art therapy.
- Life skills therapy focusing on practical skills for independent living.
- Medication management with a psychiatrist.
As you progress, the focus shifts to aftercare planning to ensure a gradual transition to independence, equipping you with the tools to thrive.
How to Find and Support Dual Diagnosis Help
Finding the right dual diagnosis help can feel overwhelming, but resources are available. Supporting a loved one also requires empathy, patience, and education.
For those supporting a loved one, remember to:
- Be Empathetic and Patient: Understand that dual diagnosis is a complex illness, not a choice. Recovery is a process with potential setbacks.
- Set Healthy Boundaries: Protect your own well-being and avoid enabling behaviors.
- Encourage Treatment Gently: Share information and express concern without using ultimatums or shame.
- Educate Yourself: Learning about dual diagnosis helps you provide better support. Our article on Supporting a loved one with mental health challenges offers more guidance.
How to Find a Dual Diagnosis Treatment Center
Finding a specialized dual diagnosis help center in New Jersey or New York is manageable with the right resources.
- Use Online Locators: The SAMHSA Treatment Locator is a comprehensive tool to find facilities by location, service, and payment options.
- Ask for Referrals: Your primary care physician or a mental health professional can provide referrals to reputable programs.
- Verify Insurance: Before committing, understand your coverage. We offer assistance to Verify Insurance to make treatment accessible.
- Ask Questions: When contacting a potential facility, ask:
- Do you offer integrated treatment for dual diagnosis?
- What therapies do you use (CBT, DBT, trauma-informed)?
- Do you provide medication management and different levels of care (PHP, IOP)?
- What does aftercare planning involve?
- What is the cost, and what insurance do you accept?
- Contact the NAMI HelpLine: The National Alliance on Mental Illness (NAMI) offers a free peer-support service and can help you find local resources via their NAMI HelpLine.
Prioritize facilities that explicitly offer integrated treatment for dual diagnosis.
The Importance of Specialized Dual Diagnosis Help for Loved Ones
Supporting a loved one with a dual diagnosis is a journey that requires resources for caregivers, too. It’s vital for family members to avoid enabling behaviors, participate in family therapy programs, and prioritize their own self-care.
Finding your own support is also crucial. Groups like Al-Anon and Nar-Anon provide a safe space for families and friends of those with addiction to share experiences and learn coping strategies. These groups emphasize that while you can’t control another person’s illness, you can find your own peace and become a powerful force for positive change.
Conclusion: Taking the First Step Toward Integrated Healing
We’ve seen that dual diagnosis—the combination of a mental health condition and a substance use disorder—requires a specialized, integrated approach. The core message is one of hope: recovery is possible. With the right dual diagnosis help, individuals can break the cycle of co-occurring struggles and find stability and purpose.
At True Life Care Mental Health, we are committed to providing this specialized care in New Jersey. Our holistic approach, flexible programs (PHP and IOP), and expert psychiatric team are designed to empower you for long-term well-being. We address the whole person, fostering resilience for life’s challenges.
If you or a loved one are struggling, you are not alone. Taking the first step is a brave, life-changing decision.
Learn more about our dual diagnosis treatment program and find out how we can support your path to recovery.