What You Need to Know About Anxiety Disorder Medication Management
Anxiety disorder medication management is the ongoing process of selecting, monitoring, and adjusting medications to effectively treat anxiety — while minimizing side effects and supporting long-term recovery.
Here’s a quick overview of how it works:
| Step | What It Involves |
|---|---|
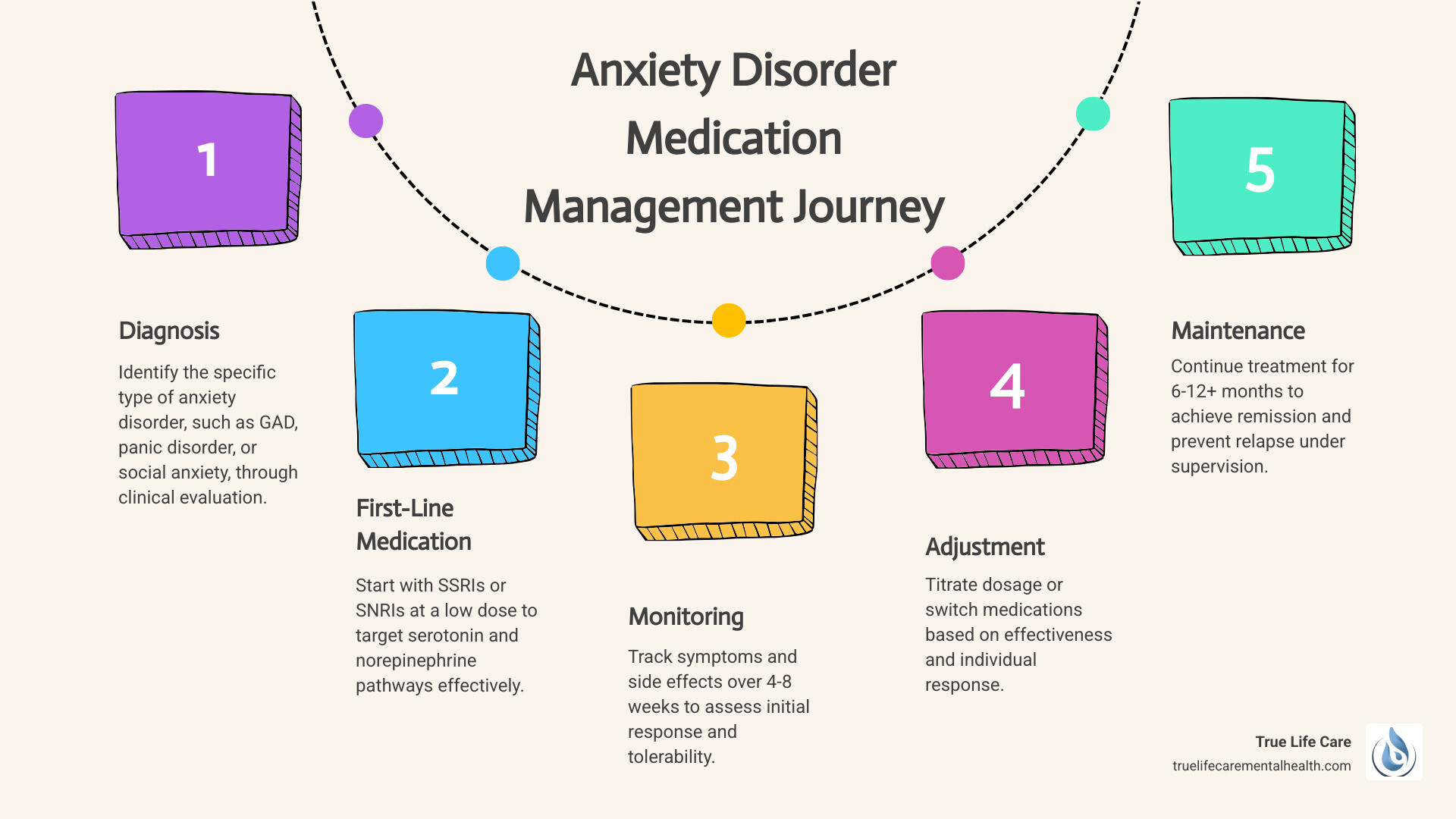
| Diagnosis | Identifying the type of anxiety disorder (GAD, panic disorder, social anxiety, etc.) |
| First-line medication | Usually an SSRI or SNRI prescribed at a low starting dose |
| Monitoring | Tracking symptoms and side effects over 4-8 weeks |
| Adjustment | Dose changes or medication switches if needed |
| Maintenance | Continuing treatment for 6-12+ months to prevent relapse |
| Tapering | Slowly reducing medication under doctor supervision when appropriate |
Anxiety disorders are among the most common mental health conditions in the United States. Millions of adults live with generalized anxiety disorder (GAD), panic disorder, or related conditions — and many of them never receive adequate treatment.
The good news? With the right medication plan, most people can get meaningful relief.
But medication management isn’t a one-size-fits-all process. The right drug, the right dose, and the right timeline vary from person to person. That’s why working closely with a qualified mental health provider matters so much.
This guide walks you through everything you need to know — from first-line medications to emerging therapies — so you can make informed decisions about your care.
First-Line Options for Anxiety Disorder Medication Management
When we begin the journey of anxiety disorder medication management, we typically start with what medical professionals call “first-line” treatments. These are the medications that have the strongest evidence for safety and effectiveness across large populations.
For most people struggling with Generalized Anxiety Disorder (GAD) or Panic Disorder (PD), the gold standard involves two classes of antidepressants: Selective Serotonin Reuptake Inhibitors (SSRIs) and Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs). While they were originally developed to treat depression, they are incredibly effective at “calming” the overactive neural pathways associated with anxiety.
| Medication Class | Common Examples | Primary Neurotransmitters Targeted | Best For |
|---|---|---|---|
| SSRIs | Escitalopram, Sertraline, Paroxetine | Serotonin | GAD, Panic Disorder, Social Anxiety |
| SNRIs | Venlafaxine, Duloxetine | Serotonin & Norepinephrine | GAD, Social Anxiety, Chronic Pain + Anxiety |
SSRIs (Selective Serotonin Reuptake Inhibitors)
SSRIs work by increasing the levels of serotonin in the brain. Serotonin is often called the “feel-good” chemical, but in the context of anxiety, it acts more like a stabilizer. It helps regulate mood, sleep, and the “fight or flight” response. By preventing the reabsorption (reuptake) of serotonin, these medications allow more of it to be available to transmit messages between neurons. This process helps the brain’s emotional processing center, the amygdala, become less reactive to perceived threats.
SNRIs (Serotonin-Norepinephrine Reuptake Inhibitors)
SNRIs go a step further by affecting both serotonin and norepinephrine. Norepinephrine is a chemical that plays a role in the body’s stress response and alertness. For some of us, especially those whose anxiety is accompanied by physical lethargy or chronic pain, SNRIs can be a game-changer. According to Scientific research on GAD and PD management, both SSRIs and SNRIs are considered first-line pharmacological treatments because of their favorable risk-to-benefit ratio.
Understanding Timelines and Dosages
One of the most important things we tell our clients in New Jersey is that anxiety disorder medication management is a marathon, not a sprint. Unlike a headache pill that works in twenty minutes, anxiety medications require time to physically change the way your brain chemistry functions.
- Initial Response: You might start to feel “different” within the first week or two, but this is often just the brain adjusting.
- Effectiveness Timeline: It typically takes 4 to 8 weeks to see the full therapeutic effect.
- Dosage Titration: We usually start at a very low “sub-therapeutic” dose to let your body adjust, then slowly increase it (titrate) until we find the “sweet spot” where symptoms vanish but side effects remain minimal.
- Remission Rates: While many people see significant improvement with the first medication they try, some may need to switch brands or classes. The goal is complete remission—where anxiety no longer interferes with your daily life.
The Role of Benzodiazepines
You’ve likely heard of medications like Xanax, Valium, or Ativan. These are benzodiazepines. They work very differently from SSRIs. While SSRIs are like a thermostat that regulates the temperature over time, benzodiazepines are like a fire extinguisher. They provide immediate, sedative relief by enhancing the effect of GABA, a neurotransmitter that slows down the central nervous system.
While they are powerful tools, we use them with extreme caution in anxiety disorder medication management.
- Short-term use: They are best used for acute panic attacks or as a “bridge” while waiting for an SSRI to kick in.
- Tolerance risks: The body can quickly become accustomed to them, meaning you need higher doses to get the same effect.
- Withdrawal symptoms: Stopping them abruptly can be dangerous and lead to “rebound anxiety” that is worse than the original symptoms.
As noted in Scientific research on benzodiazepine risks, long-term use is generally discouraged due to the potential for dependence and cognitive impairment, particularly in older adults.
Managing Side Effects and Treatment Duration
Once we find a medication that works, the next phase of anxiety disorder medication management focuses on sustainability. We want you to feel better, but we also want you to be able to live your life without being hindered by the treatment itself.
Navigating Anxiety Disorder Medication Management Side Effects
Every body is different. What makes one person feel great might make another feel “off.” Most side effects occur in the first two weeks and then subside as the body reaches “steady state.”
- Nausea and GI Upset: Common in the first few days. Taking medication with food usually helps.
- Jitteriness: Sometimes, an SSRI can feel a bit “stimulating” at first, almost like too much caffeine. This usually passes.
- Sexual Side Effects: This is a common concern. If you experience a change in libido or performance, don’t be embarrassed to tell us. We can often adjust the dose or add a secondary medication to counteract this.
- Weight Gain: Some medications are more “weight-neutral” than others. Monitoring your diet and staying active can help, but if the scale keeps moving, we can look at alternative options.
- Insomnia: If your medication makes you feel alert, we might suggest taking it in the morning. If it makes you drowsy, we switch it to bedtime.
The golden rule of anxiety disorder medication management is: Never suffer in silence. If a side effect is bothering you, a consultation with your doctor can often solve the problem with a simple adjustment.
Monitoring Treatment Response
How do we know if it’s working? We don’t just guess. We use symptom tracking and clinical monitoring. We look for:
- A decrease in the frequency of panic attacks.
- Less “racing thoughts” at night.
- An easier time socializing or going to work.
- Improved sleep quality.
Statistically, medication adherence is the biggest hurdle. Many people stop taking their meds because they feel better (and think they don’t need them) or because they feel worse in the first week. We are here to help you navigate those bumps so you can reach the maintenance phase.
Maintenance and Relapse Prevention
Once you feel “back to yourself,” we usually recommend staying on the medication for at least 6 to 12 months. This is known as the maintenance phase. It allows your brain to solidify its new, healthier patterns. Think of it like a cast for a broken bone—you don’t take the cast off the second the pain stops; you wait for the bone to fully heal. Stopping too early is the number one cause of relapse.
Alternative, Emerging, and Holistic Therapies
Sometimes, first-line medications aren’t the right fit, or they need a little help. In these cases, anxiety disorder medication management expands to include secondary medications and lifestyle interventions.
- Buspirone: A unique anti-anxiety medication that isn’t a sedative and isn’t an antidepressant. It’s often used as an “add-on” for GAD.
- Beta-blockers: (Like Propranolol) These don’t stop the feeling of anxiety in your head, but they stop the physical symptoms like a racing heart or shaky hands. They are favorites for public speakers and performers.
- Hydroxyzine: An antihistamine (similar to Benadryl but stronger) that can be used “as needed” for anxiety without the addiction risks of benzodiazepines.
The Role of Psychotherapy and Lifestyle
We believe in a holistic approach. Medication manages the chemistry, but therapy manages the “software.” Cognitive Behavioral Therapy (CBT) is the most effective partner for medication. It teaches you how to challenge the thoughts that trigger the anxiety in the first place.
Furthermore, we cannot overstate the importance of movement. Scientific research on exercise for anxiety shows that regular physical activity can be just as effective as some medications for mild to moderate anxiety. It burns off excess cortisol and boosts natural endorphins.
The Future of Anxiety Disorder Medication Management
The field of psychiatry is currently exploding with new research into “rapid-acting” treatments for those who don’t respond to traditional meds.
- Ketamine: Originally an anesthetic, low-dose intravenous ketamine has shown remarkable results for treatment-resistant depression and anxiety. According to Scientific research on Ketamine for mental health, it can provide relief within hours rather than weeks.
- Psychedelic-Assisted Therapy: Research into psilocybin and MDMA (under strict clinical supervision) is showing promise for severe PTSD and social anxiety. As Scientific research on psychedelic therapy suggests, these substances may help “reset” the brain’s emotional processing centers. While these aren’t standard “at-home” medications yet, they represent the future of the field.
Considerations for Special Populations
Anxiety disorder medication management must be personalized, especially for:
- Geriatric Care: Older adults process medication differently and are more sensitive to side effects like dizziness (which can lead to falls).
- Maternal Health: For our neighbors in New Jersey who are pregnant or breastfeeding, we carefully weigh the risks of untreated anxiety against the potential impact of medication on the baby.
- Addiction History: For those in recovery, we strictly avoid benzodiazepines and focus on non-habit-forming options like SSRIs, Buspirone, or Gabapentin.
Frequently Asked Questions about Anxiety Medication
How long does it take for anxiety medication to work?
As we mentioned, it’s not instant. While you might feel some sedative effects from certain drugs (like hydroxyzine or benzos) immediately, the heavy lifters like SSRIs and SNRIs take 4 to 8 weeks to reach their full potential. You might feel worse before you feel better—hang in there!
Can I stop taking my medication once I feel better?
Please, don’t do this without talking to us first! Stopping abruptly can cause “discontinuation syndrome,” which feels like a bad flu combined with a surge of anxiety. If it’s time to stop, we will help you “taper” (slowly reduce the dose) over several weeks to keep your brain stable.
What are the risks of long-term benzodiazepine use?
The primary risks are dependency, tolerance, and cognitive “fog.” Over time, they can also interfere with your sleep architecture (preventing deep REM sleep) and increase the risk of falls or memory issues as you age. They are excellent “rescue” meds, but poor “everyday” meds.
Conclusion
At True Life Care Mental Health, we understand that seeking help for anxiety is a big step. Whether you are in Bergen County, Morris County, or right in the heart of NYC, our goal is to provide a supportive, judgment-free environment where you can find the relief you deserve.
Our approach to anxiety disorder medication management is rooted in science but delivered with heart. We don’t just hand out prescriptions; we offer a holistic, evidence-based care model that includes expert psychiatric care, flexible programs like PHP and IOP, and a deep commitment to your long-term recovery.
From the quiet suburbs of Clinton and Boonton to the busy streets of Clifton and Fair Lawn, we are proud to serve the New Jersey community. We believe in empowering you with the tools, the knowledge, and the personalized treatment plan necessary to reclaim your life from anxiety.
If you’re ready to start your journey toward wellness, we are here to walk with you every step of the way. Your recovery isn’t just a goal—it’s our mission.