Schizophrenia Treatment in New Jersey: What You Need to Know

Schizophrenia treatment in New Jersey is available across a wide range of care levels, from inpatient stabilization to outpatient therapy, with programs designed to treat the whole person — not just the symptoms.
Quick answer — here are the main treatment options available in NJ:
- Inpatient care – Short-term stabilization for acute episodes
- Residential treatment – Structured, longer-term support in a live-in setting
- Partial Care Programs (PHP) – Full-day treatment, 5 days a week
- Intensive Outpatient Programs (IOP) – Flexible treatment, 3–5 days a week
- Outpatient therapy – Ongoing medication management and counseling
- Dual diagnosis programs – Integrated care for co-occurring substance use
- Community support programs – Family education, peer support, and vocational rehab
Schizophrenia is a chronic brain condition that makes it hard to tell what is real from what isn’t. It affects how a person thinks, feels, and behaves — and it can be deeply disruptive to everyday life.
It typically begins in the late teens or early twenties. Without the right support, it can lead to job loss, housing instability, and social isolation.
The good news? With early intervention and the right treatment plan, schizophrenia is manageable. Most people can lead meaningful, connected lives with consistent care.
This guide walks you through everything you need to know about finding effective schizophrenia treatment in New Jersey — from understanding symptoms to navigating insurance and finding the right level of care.
Schizophrenia Treatment in New Jersey terms explained:
- Bipolar Disorder Therapy in New Jersey
- Psychiatric Care in Monmouth County NJ
- Mental Health Telehealth IOP in New Jersey
Understanding Schizophrenia Symptoms and Diagnosis
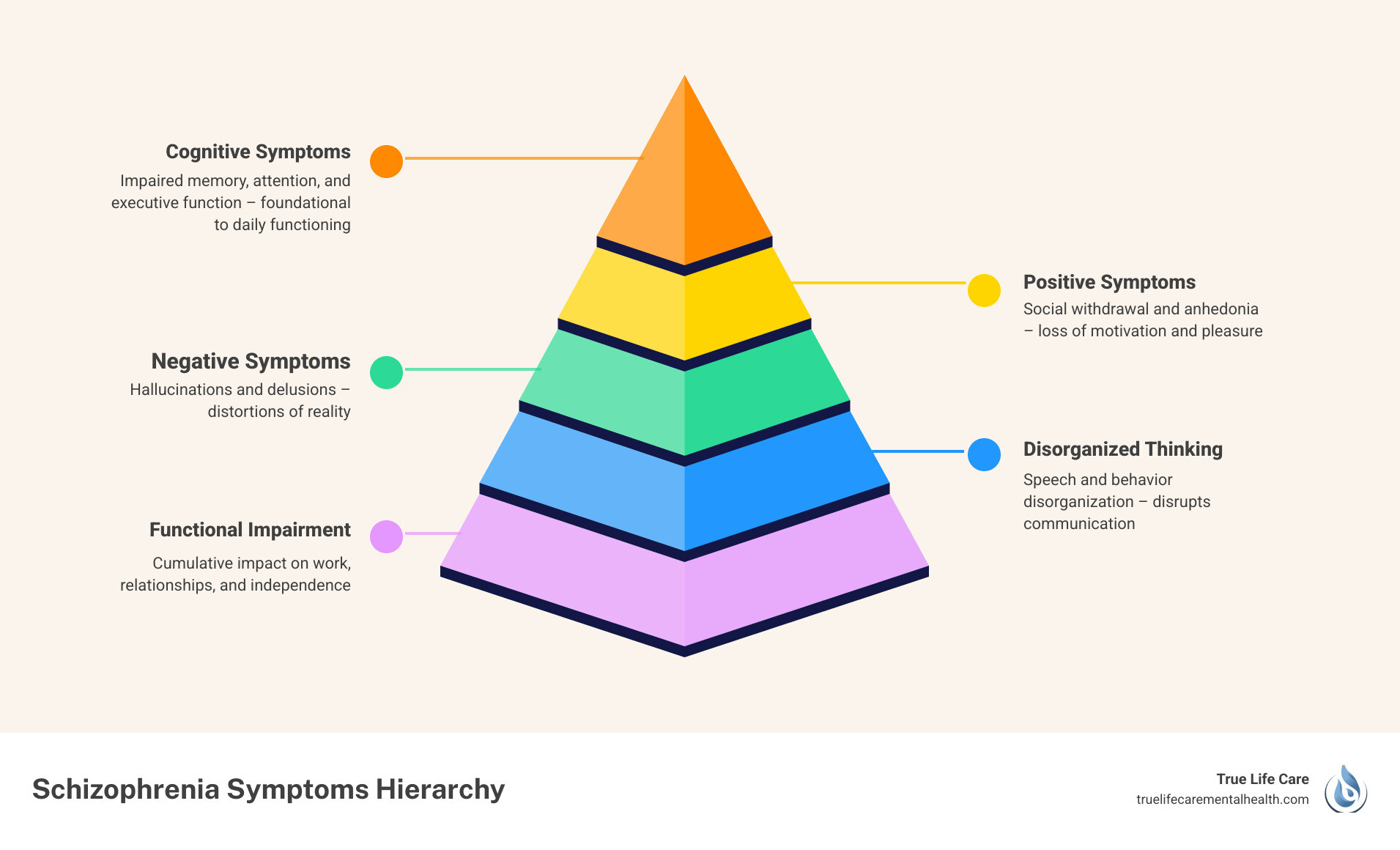
To find the right Schizophrenia Treatment in New Jersey, we first have to understand how the condition manifests. Schizophrenia isn’t a “one-size-fits-all” disorder; symptoms are generally categorized into three main groups: positive, negative, and cognitive.
Positive Symptoms
“Positive” doesn’t mean “good” in this context; it refers to behaviors that are added to a person’s experience. These are often the most visible signs of schizophrenia:
- Hallucinations: Hearing voices or seeing things that others don’t. These can range from fleeting shadows to vivid, demanding images.
- Delusions: Strong beliefs that aren’t based in reality, such as believing one has special powers or that others are plotting against them.
- Disorganized Thinking: Difficulty organizing thoughts or connecting them logically, which often leads to jumbled speech.
Negative Symptoms
These involve a “taking away” or a loss of normal functions. They can sometimes be mistaken for clinical depression:
- Social Withdrawal: Pulling away from friends and family.
- Anhedonia: A loss of interest in activities once enjoyed.
- Flat Affect: Showing very little emotional expression through facial movements or tone of voice.
Cognitive Symptoms
These symptoms affect the brain’s “operating system” and can make daily life incredibly challenging:
- Executive Functioning Issues: Trouble processing information to make decisions.
- Memory Deficits: Difficulty using information immediately after learning it (working memory).
Understanding these distinctions is vital, especially when comparing schizophrenia to related conditions like schizoaffective-disorder, which includes a significant mood component like mania or depression.
Differentiating Psychotic Disorders
It is common to confuse different psychotic disorders. Our diagnostic process in New Jersey involves careful evaluation to ensure the right path forward.
| Feature | Schizophrenia | Schizoaffective Disorder | Schizoid Personality Disorder |
|---|---|---|---|
| Primary Symptoms | Hallucinations, delusions, disorganized speech | Psychosis plus major mood episodes (mania/depression) | Social detachment and limited emotional range |
| Reality Perception | Significantly impaired | Impaired during psychotic episodes | Usually intact; no hallucinations/delusions |
| Duration | Symptoms must last at least 6 months | Ongoing, with mood episodes present much of the time | Pervasive pattern starting in early adulthood |
| Treatment Focus | Antipsychotics and psychosocial support | Antipsychotics plus mood stabilizers/antidepressants | Primarily talk therapy for social skills |
Schizophrenia Treatment in New Jersey: Levels of Care

When seeking Schizophrenia Treatment in New Jersey, the “level of care” refers to how much support and supervision a person needs. In our state, we have a robust network of mental health facilities in New Jersey offering various intensities of care.
- Inpatient Stabilization: This is the highest level of care, usually occurring in a hospital. Stays typically last 5 to 12 days and focus on keeping the individual safe during an acute crisis.
- Residential Treatment: For those who need more than a few days, residential programs offer a structured environment (often 30 to 42 days) where patients live on-site and participate in intensive therapy.
- Partial Care Programs (PHP): These mental health programs in New Jersey are “day programs.” Patients attend treatment for about 6 hours a day, 5 days a week, but return home in the evenings.
- Intensive Outpatient Programs (IOP): A step down from PHP, IOP usually requires 3 to 5 days of attendance for 2 to 3 hours per session. It’s ideal for those transitioning back to work or school.
- Outpatient Medication Management: This involves regular visits to a psychiatrist to monitor the effectiveness of antipsychotic medications and manage side effects.
Early Signs and Schizophrenia Treatment in New Jersey
Early intervention is perhaps the single most important factor in long-term success. Approximately 100,000 young adults in the U.S. experience their first episode of psychosis each year, with peak onset occurring between ages 15 and 25.
Early signs often include social withdrawal, a drop in academic performance, or unusual suspiciousness. In New Jersey, specialized programs like Coordinated Specialty Care – Community Integration (CSC-CI) focus on these “first-episode” cases. Research from institutions like Rutgers New Jersey Medical School emphasizes that treating psychosis within the first two years of onset significantly improves the lifetime trajectory of the illness.
Dual Diagnosis: Addressing Co-occurring Substance Use
It is a sobering reality that schizophrenia and substance use often go hand-in-hand. In fact, 59% of New Jersey adults who attended treatment in 2022 were diagnosed with a co-occurring disorder.
Many individuals with schizophrenia attempt to “self-medicate” to quiet the noisy thoughts or hallucinations they experience. They might use cannabis or alcohol to calm down, but these substances often worsen underlying psychosis. Furthermore, adults with schizophrenia are disproportionately more likely to be represented in opioid-related ER visits.
The overlap in brain chemistry — specifically the role of dopamine in the brain’s reward centers — makes this combination particularly dangerous. Effective mental health treatments in New Jersey must use an integrated model. This means treating the addiction and the schizophrenia simultaneously, rather than sequentially. If you only treat one, the other is likely to cause a relapse.
Family Support and Community Resources in NJ
Schizophrenia doesn’t just affect the individual; it affects the entire family. Caregiver burnout is real, and having a support system is essential for the long-term wellness of everyone involved.
New Jersey offers Intensive Family Support Services (IFSS), a state-wide program available in counties like Bergen, Mercer, and Warren. These programs provide:
- Family support groups
- Respite care
- Psychoeducation about the illness
- Advocacy and referral services
For individuals who struggle to stay engaged with treatment due to anosognosia (a condition where a person is unaware they have a disability), New Jersey utilizes Assisted Outpatient Treatment (AOTS). This is a form of involuntary outpatient commitment (IOC) designed to provide a structured, court-monitored framework for care, ensuring the individual receives medication and support even if they lack the insight to seek it themselves.
You can find a full directory of NJ Mental Health and IFSS Programs to see what is available in your specific county.
Accessing Schizophrenia Treatment in New Jersey via Medicaid
Navigating the financial side of care can be daunting. Fortunately, top outpatient mental health services in New Jersey often accept a variety of insurance plans.
NJ FamilyCare (Medicaid) generally covers:
- Clinical assessments
- Antipsychotic medications
- Inpatient stabilization
- PHP and IOP services
The key is documenting “medical necessity.” If a doctor determines that treatment is required to prevent a crisis or maintain stability, coverage is typically approved. For those in immediate need, the 988 Suicide & Crisis Lifeline provides 24/7 support and can help link you to local emergency services.
Holistic and Evidence-Based Treatment Approaches
While medication is the cornerstone of Schizophrenia Treatment in New Jersey, it is rarely enough on its own. We believe in a holistic approach that combines traditional medicine with modern therapeutic techniques.
- Antipsychotic Medications: These help balance dopamine levels in the brain to reduce hallucinations and delusions.
- Cognitive Behavioral Therapy for psychosis (CBTp): This helps individuals identify and change the thought patterns that lead to distress.
- Social Skills Training: Many people with schizophrenia struggle with social cues; this training helps them rebuild the skills needed for work and relationships.
- Holistic Complements: Approaches such as yoga, acupuncture, and even Omega-3 fatty acid supplementation have shown promise in supporting brain health and reducing the “negative” symptoms of the disorder.
For more on how these services are integrated, see our guide on adult mental health services in New Jersey.
Frequently Asked Questions about Schizophrenia
Is schizophrenia a genetic condition?
Yes, there is a strong hereditary component. If a close relative has schizophrenia, your risk is higher. However, genetics aren’t the whole story. Environmental triggers — such as high stress or substance use during brain development — and imbalances in brain chemistry (like dopamine and glutamate) also play significant roles.
Can schizophrenia be managed without medication?
In almost all cases, antipsychotic medication is necessary to manage the biological aspects of the condition. However, medication works best when paired with a holistic integration of therapy, family support, and lifestyle changes. Treating it as a “whole-person” issue leads to much better long-term wellness.
What is the difference between schizophrenia and schizoaffective disorder?
The main difference lies in the presence of mood symptoms. While someone with schizophrenia may feel depressed, someone with schizoaffective disorder meets the full diagnostic criteria for a mood disorder (like Bipolar Disorder or Major Depressive Disorder) in addition to the criteria for schizophrenia.
Conclusion
At True Life Care Mental Health, we understand that a diagnosis of schizophrenia can feel overwhelming. But it is not the end of the story. By utilizing personalized recovery plans and evidence-based care, we help individuals across New Jersey — from Bergen to Warren County — reclaim their lives.
Whether you are looking for a Partial Care Program or need help navigating a dual diagnosis, we are here to provide the expert psychiatric care and warm, supportive environment you deserve.
Start your journey with Schizophrenia Treatment in New Jersey today and take the first step toward long-term well-being.