The Reality of Seeking Intensive Help for Bipolar Mood Disorders
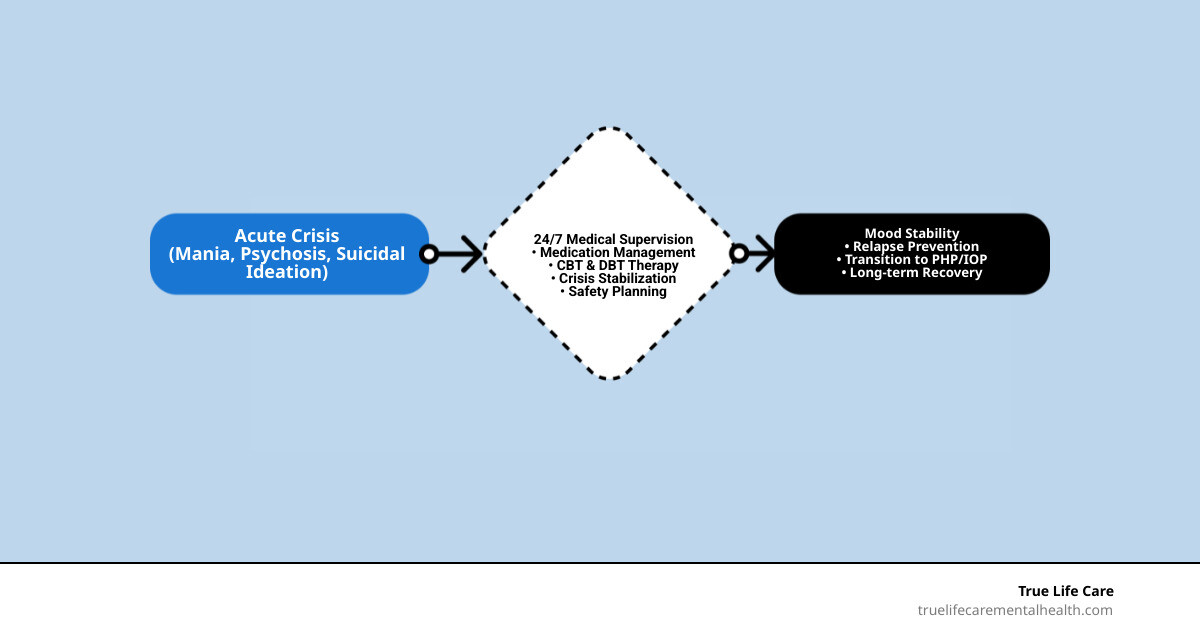
Inpatient programs for bipolar disorder represent the highest level of clinical intervention for individuals navigating the turbulent cycles of mania and depression. These programs are structured, 24/7 supervised treatment settings designed to stabilize severe mood episodes — including mania, psychosis, and suicidal depression — when outpatient care is no longer sufficient to ensure safety or clinical progress. At True Life Care in Matawan, NJ, we help adults in Monmouth County and across New Jersey access intensive psychiatric support during some of the most vulnerable moments of their lives. We also assist during psychiatric emergencies, offering a safe, clinically supervised setting where healing can begin immediately. True Life Care is an out-of-network provider and accepts PPO plans, ensuring that patients receive specialized, high-acuity care tailored to their unique neurobiological needs.
Bipolar disorder is not merely a series of “mood swings”; it is a complex biological condition that affects the brain’s ability to regulate energy, sleep, and executive function. When a person enters a state of acute mania or profound depression, the prefrontal cortex — the part of the brain responsible for decision-making and impulse control — can become significantly impaired. Inpatient care provides an external “regulatory system” for the patient, offering the structure and safety that the brain cannot currently provide for itself.
Who needs inpatient bipolar care?
- Acute Manic Episodes: Individuals experiencing a manic episode that puts themselves or others at risk. This is often characterized by impulsive spending, reckless behavior, hypersexuality, or a total lack of sleep for several days, which can lead to physical exhaustion and cardiovascular strain.
- Severe Depressive States: Individuals with persistent suicidal ideation or severe depressive episodes where they can no longer maintain their own safety, basic hygiene, or nutritional intake.
- Treatment Resistance: Those not responding to outpatient medication or therapy, indicating a need for a more controlled environment to adjust clinical protocols and monitor pharmacological responses in real-time.
- Psychotic Features: Anyone experiencing psychosis alongside bipolar symptoms, such as hallucinations (hearing or seeing things that aren’t there) or delusions (fixed false beliefs) that distort reality and increase the risk of accidental harm.
- Functional Collapse: People unable to perform basic self-care due to extreme mood instability, including those who have stopped eating, drinking, or communicating with their support systems.
What does inpatient bipolar treatment include?
- 24/7 Medical Supervision: Constant psychiatric monitoring to ensure safety and immediate intervention during rapid mood shifts or the emergence of side effects.
- Advanced Medication Management: Evaluation and adjustment of mood stabilizers, antipsychotics, and antidepressants, often utilizing advanced tools like pharmacogenomics to find the right fit for the patient’s genetic profile.
- Evidence-Based Modalities: Intensive application of Cognitive Behavioral Therapy (CBT) and Dialectical Behavior Therapy (DBT) specifically tailored for mood regulation and distress tolerance.
- Group Therapy and Psychoeducation: Helping patients understand the biological roots of their disorder, such as the role of neurotransmitters like dopamine and serotonin, and beginning the healing process within a supportive community.
- Specialized Care for Comorbidities: Focused treatment for bipolar depression, schizophrenia-spectrum symptoms, and co-occurring psychiatric concerns like anxiety or substance use disorders.
- Crisis Stabilization and Safety Planning: Developing a robust plan to manage future triggers and prepare for the challenges of the outside world.
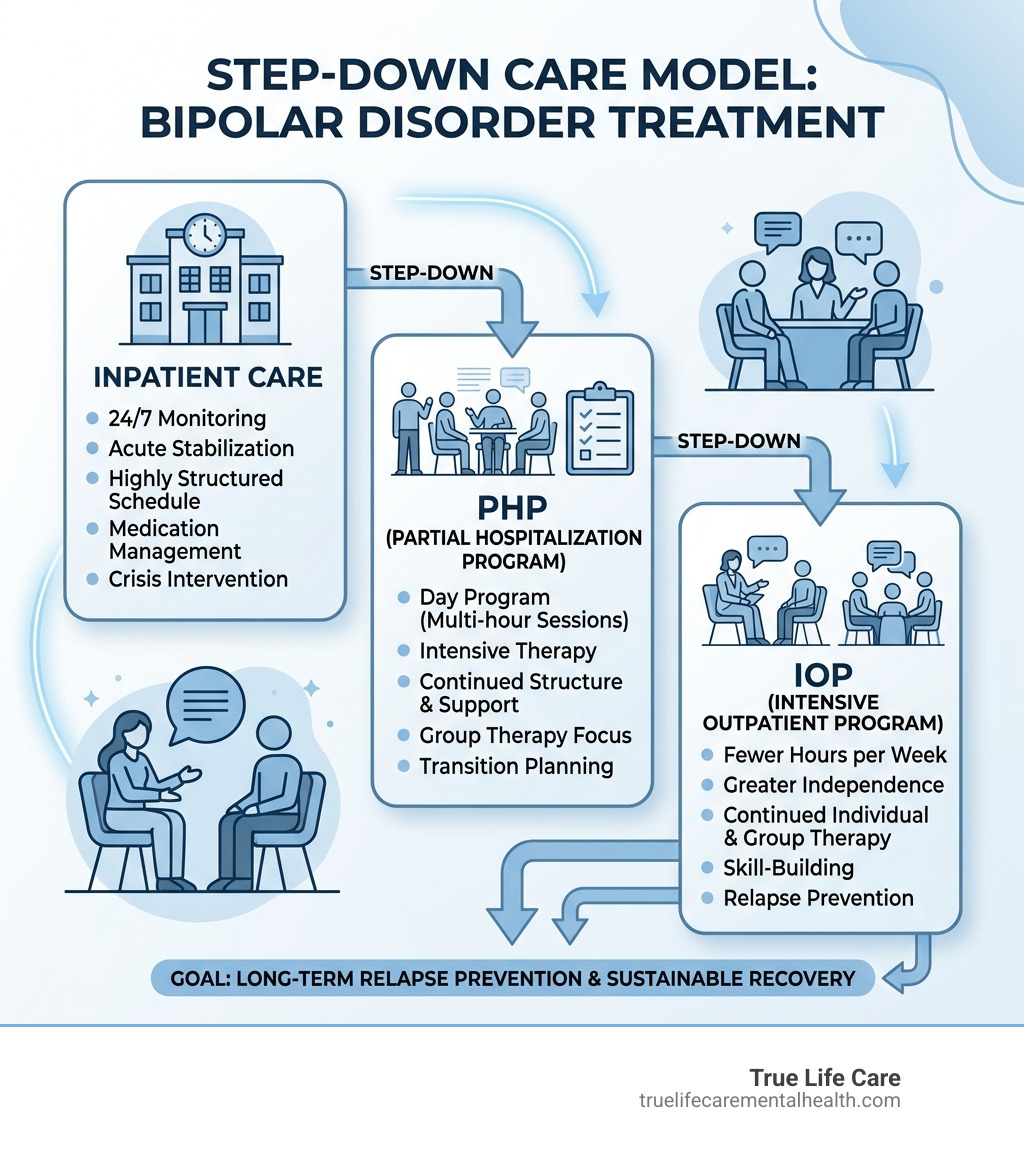
- Comprehensive Aftercare Planning: Coordinating a seamless step-down to Partial Hospitalization Programs (PHP) or Intensive Outpatient Programs (IOP) to maintain the gains made during the inpatient stay.
How long does it last? Most acute inpatient stays range from 5 to 14 days, depending on symptom severity and the speed of stabilization. However, the inpatient phase is just the beginning. Residential programs or high-intensity PHP can extend to six weeks or longer for more complex cases where long-term behavioral changes and neurochemical stabilization are required.
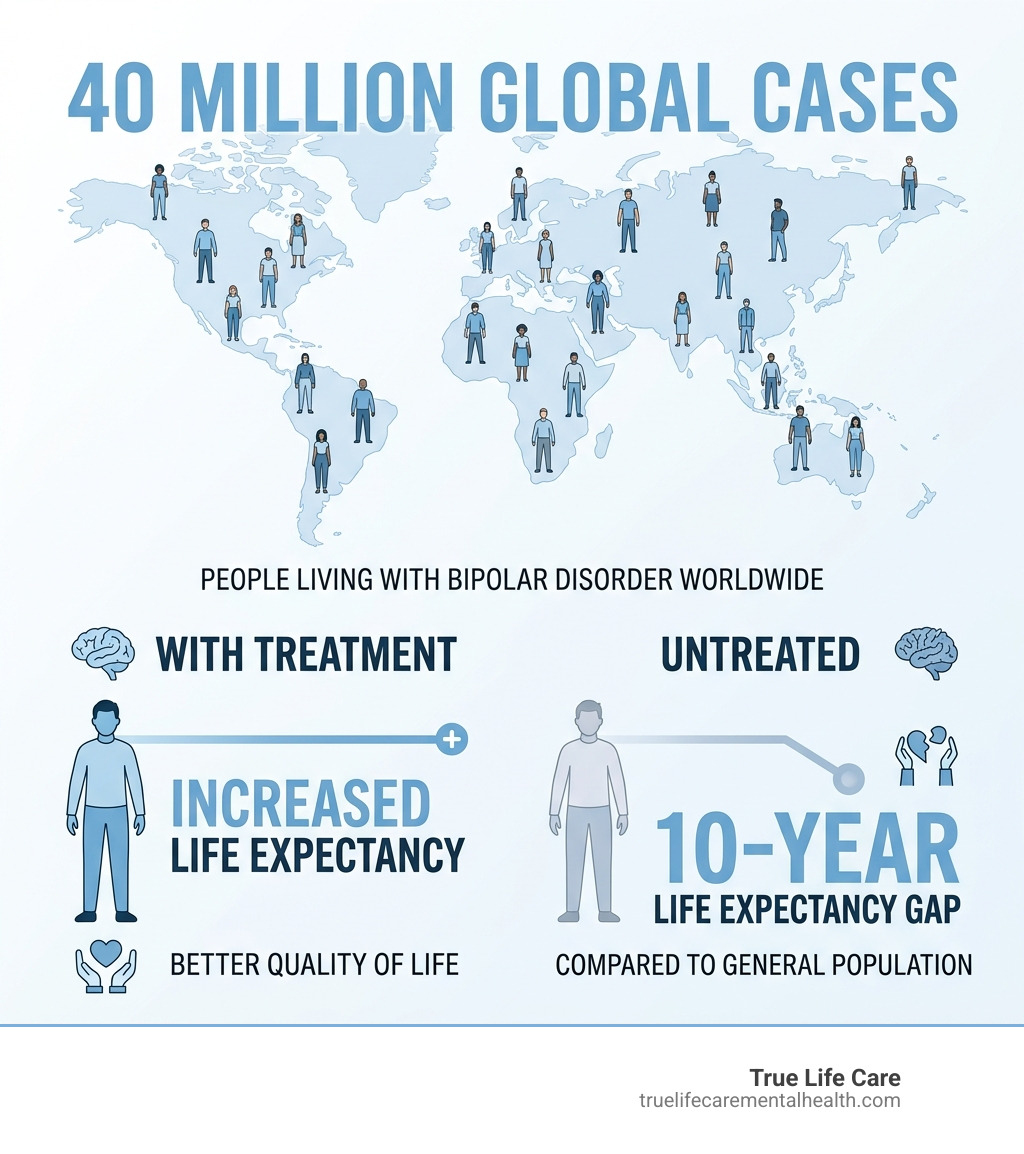
More than 40 million people worldwide live with bipolar disorder, according to the World Health Organization — and for a significant portion of them, the path to stability will at some point run through an inpatient program. At True Life Care, we serve adults across Monmouth County and throughout New Jersey from our Matawan, NJ location, with a strong focus on group therapy, healing, depression treatment, and support for patients experiencing psychosis or schizophrenia-related symptoms. Whether it is a first episode of mania or a long pattern of cycling moods, the decision to pursue inpatient care is a brave and necessary step toward reclaiming one’s life.
True Life Care is an out-of-network provider and accepts PPO plans, helping individuals and families access specialized psychiatric care in New Jersey. This guide lays out 10 hard lessons that patients, families, and clinicians have learned about inpatient bipolar programs — lessons about what works, what to expect, how group-based healing supports recovery, and how to build stability after a psychiatric emergency.
Similar topics to inpatient programs for bipolar disorder:
Understanding the Spectrum: Bipolar I, II, and Cyclothymia
One of the most difficult lessons we learn is that bipolar disorder is not a single, uniform experience. It is a spectrum of intensity, often referred to as the “Bipolar Spectrum.” When we talk about inpatient programs for bipolar disorder, the treatment protocol depends heavily on which specific type of the disorder is present. Understanding these nuances is essential for effective healing and long-term management.
- Bipolar I Disorder: This is the most severe form, defined by manic episodes that last at least seven days, or by manic symptoms that are so severe that the person needs immediate hospital care. Usually, depressive episodes occur as well, typically lasting at least two weeks. In Bipolar I, the mania can be so intense that it leads to a total break from reality (psychosis), requiring antipsychotic intervention and a highly secure environment.
- Bipolar II Disorder: This is defined by a pattern of depressive episodes and hypomanic episodes, but not the full-blown manic episodes that are typical of Bipolar I. While “hypomania” sounds less severe, the instability can be just as disruptive. People with Bipolar II often spend more time in deep, debilitating depression, which carries a high risk of suicidal ideation and requires specialized depression treatment.
- Cyclothymic Disorder (Cyclothymia): This involves periods of hypomanic symptoms as well as periods of depressive symptoms lasting for at least two years. However, the symptoms do not meet the diagnostic requirements for a hypomanic episode and a depressive episode. It is a chronic state of low-level mood cycling that still requires clinical attention to prevent it from evolving into Bipolar I or II.
Lesson 1: Diagnosis is the first step toward targeted healing.
Many people spend years being treated for “standard” depression before realizing they actually have bipolar disorder. In an inpatient setting, clinicians use the DSM-5 criteria to differentiate between these types. We look for “mixed features”—where mania and depression happen at the same time, creating a dangerous state of high energy and low mood—and “rapid cycling,” which is defined as four or more mood episodes in a 12-month period. Getting the label right isn’t about pigeonholing you; it’s about making sure the medication doesn’t accidentally trigger a manic switch. For example, prescribing an antidepressant without a mood stabilizer to someone with Bipolar I can be disastrous, potentially inducing a life-threatening manic crisis.
Daily Structure within Inpatient Programs for Bipolar Disorder
If there is one thing a manic episode hates, it is a schedule. Yet, structure is exactly what the brain needs to recalibrate. A typical day in a high-quality program involves a 14-hour daily structured schedule. This isn’t just to keep you busy; it’s to restore a natural rhythm to a body that has likely been deprived of sleep and routine. The brain’s circadian rhythms—the internal clock that regulates sleep-wake cycles—are often deeply disrupted in bipolar disorder. The inpatient environment acts as an external regulator, using light, activity, and meal times to reset the biological clock.
Lesson 2: Structure provides the safety mania often destroys.
In a bipolar disorder inpatient rehab, the routine includes regular meal times, medication rounds, multiple group therapy sessions, and monitored sleep periods. This 24/7 monitoring ensures that as medications are adjusted, any side effects or shifts in mood are caught immediately by nursing staff. This level of oversight is impossible in an outpatient setting, making the inpatient environment the safest place for acute stabilization. By removing the chaos of daily life, the patient can focus entirely on the internal work of stabilization.

When Inpatient Programs for Bipolar Disorder Become Necessary
Knowing when to transition from outpatient therapy to a full inpatient program is a critical skill for patients and their families. Often, the “lesson” here is learned in the middle of a crisis, but it doesn’t have to be. We generally recommend bipolar disorder treatment in Monmouth County when safety is at risk or when the complexity of the symptoms exceeds the capacity of weekly therapy. From our Matawan, NJ location, we help Monmouth County residents and individuals throughout New Jersey access timely psychiatric support when symptoms escalate quickly.
Lesson 3: Recognizing a psychiatric emergency is a life-saving skill.
A psychiatric emergency isn’t always a dramatic event; sometimes it is a quiet, profound withdrawal. It can look like:
- Psychosis: Losing touch with reality, hearing voices, or experiencing delusions. This is common in severe Bipolar I and may also overlap with schizophrenia-spectrum disorders, requiring immediate medical intervention to prevent harm to the self or others.
- Inability to function: Not eating, not sleeping for days, or being unable to maintain basic hygiene. When the body begins to break down physically due to the metabolic demands of mania or the neglect of depression, the mind cannot heal.
- Medication Non-compliance: When someone stops taking mood stabilizers, leading to a rapid and dangerous spiral. Inpatient care allows for a controlled re-introduction of necessary medications under constant observation.
- Suicidal Ideation: When the “lows” of bipolar depression become life-threatening. This is a critical emergency that requires 24/7 supervision and a secure environment.
- Severe depressive shutdown: Profound hopelessness, withdrawal, slowed movement (psychomotor retardation), or inability to perform daily tasks can signal a need for immediate depression treatment in a supervised setting.
In our Matawan, NJ location, we help residents navigate these emergencies by providing a safe landing spot for acute stabilization. Safety planning starts the moment you walk in, ensuring that the immediate threat is neutralized so the long-term work of healing can begin. We focus on de-escalation, clinical support, and compassionate intervention so patients feel supported rather than confined during psychiatric emergencies. True Life Care is an out-of-network provider and accepts PPO plans, allowing us to offer a high staff-to-patient ratio for these critical moments.
Evaluating Success Rates of Inpatient Programs for Bipolar Disorder
It is a hard truth: inpatient care is not a “cure.” Bipolar disorder is a chronic condition that requires lifelong management. However, the success of a program is measured by how well it prepares you for the world outside. Success is not just the absence of symptoms during the stay; it is the presence of a robust plan for the future and the acquisition of coping skills.
Lesson 4: Success is measured by long-term management, not just immediate relief.
When choosing a bipolar treatment center, look at their aftercare planning, psychiatric follow-up, and how well they integrate therapy for bipolar depression, psychosis, schizophrenia-spectrum symptoms, and relapse prevention. High-performing programs focus on symptom reduction, emotional healing, and long-term stability. Inpatient care changes the trajectory of the disorder by providing the intensive education needed to manage the condition for decades. We teach patients to recognize their “prodromal symptoms”—the early warning signs that a mood shift is coming—so they can intervene before a full-blown crisis occurs. This proactive approach is the hallmark of successful long-term recovery.
The Core Pillars of Healing: Group Therapy and Evidence-Based Care
Isolation is the fuel that keeps bipolar episodes burning. When you are manic, you might feel “above” everyone else, leading to social friction and broken relationships; when you are depressed, you feel unworthy of others, leading to profound withdrawal. Group therapy breaks this cycle by fostering a sense of shared experience, accountability, and community-based healing. It provides a laboratory for social interaction where patients can test new coping skills in a safe environment.
Lesson 5: Healing happens in community, not isolation.
In our bipolar disorder therapy in NJ, group therapy is one of the most important parts of the daily inpatient schedule. Patients benefit from hearing how others manage bipolar depression, manic symptoms, psychosis recovery, family strain, and the shame that often follows a psychiatric crisis. This shared process supports healing by reducing stigma and helping patients realize they are not facing the disorder alone. The “therapeutic milieu”—the environment of the facility itself—becomes a place of mutual support.
We rely on several evidence-based pillars that are integrated into the daily inpatient schedule:
- CBT (Cognitive Behavioral Therapy): This helps patients identify the distorted thought patterns that trigger mood shifts. For example, “all-or-nothing” thinking can lead to a depressive spiral if a single task isn’t completed perfectly. CBT is especially useful in depression treatment because it helps patients challenge hopeless thoughts and build healthier behaviors through behavioral activation.
- DBT (Dialectical Behavior Therapy): This is essential for learning distress tolerance and emotional regulation. When a mood shift feels like an overwhelming surge, DBT provides the tools to “ride the wave” without acting on impulsive or self-destructive urges. It teaches mindfulness as a way to stay grounded in the present moment.
- Interpersonal Social Rhythm Therapy (IPSRT): This is a specialized bipolar therapy that focuses on stabilizing daily routines. By tracking sleep, meals, and social interactions, patients can stabilize their biological clocks, which is a key factor in preventing future manic or depressive episodes. IPSRT is based on the understanding that disruptions in social rhythms can trigger mood episodes in vulnerable individuals.
- Psychoeducation Groups: These sessions teach patients and families how bipolar disorder works, why medication adherence matters, and how early warning signs of mania, depression, or psychosis can be recognized before symptoms intensify. Knowledge is power in the management of a chronic illness.
- Process Groups: These therapist-led groups create space for honest discussion, emotional expression, and interpersonal feedback, all of which support deeper healing and the resolution of underlying trauma.
| Feature | CBT for Bipolar | DBT for Bipolar |
|---|---|---|
| Primary Focus | Changing negative thought patterns and cognitive distortions | Emotional regulation, distress tolerance, and mindfulness |
| Goal | Symptom reduction and identifying triggers | Managing intense emotional “surges” and improving relationships |
| Key Skill | Cognitive restructuring and behavioral activation | Mindfulness, interpersonal effectiveness, and radical acceptance |
| Application | Best for managing depressive episodes and cognitive clarity | Best for managing impulsive manic urges and emotional volatility |
High-quality inpatient care also incorporates trauma-informed treatment, relapse prevention planning, medication management, sleep stabilization, and supportive psychiatric care for patients whose symptoms overlap with schizophrenia-spectrum conditions. For many individuals, group therapy becomes the place where healing truly starts — not because symptoms disappear overnight, but because connection makes recovery feel possible again. Healing in a group setting allows patients to see their symptoms reflected in others, which reduces the shame and stigma often associated with the disorder. It provides a safe space to practice social skills, emotional regulation, communication, and trust before returning to the complexities of daily life.
Managing Complexities: Schizophrenia, Depression, and Co-occurring Disorders
Bipolar disorder rarely travels alone. In fact, research shows that a vast majority of people with bipolar disorder have at least one other mental health condition, such as an anxiety disorder, ADHD, or a substance use disorder. This complexity requires a sophisticated clinical approach that doesn’t just treat the mood swings, but addresses the whole person and their unique diagnostic profile.
Lesson 6: Bipolar rarely travels alone—addressing co-occurring schizophrenia and depression is vital.
At True Life Care, we provide comprehensive mental health care that addresses these complexities. Sometimes, bipolar symptoms overlap with schizophrenia, leading to a diagnosis of schizoaffective disorder or requiring careful assessment of schizophrenia-spectrum symptoms such as hallucinations, disorganized thinking, paranoia, or delusions. This requires a delicate balance of antipsychotic medications, mood stabilizers, and close psychiatric monitoring to ensure the patient is neither over-medicated nor under-treated.
Depression treatment is also a major part of inpatient bipolar care. Bipolar depression is distinct from unipolar depression; it can involve profound hopelessness, exhaustion, slowed thinking, suicidal ideation, withdrawal from loved ones, and a complete loss of interest in life. Because bipolar depression is often more resistant to treatment than standard depression, it requires a careful, individualized plan. We use advanced tools like pharmacogenomics (genetic testing) to see how your body processes medications. This helps inform treatment decisions, reduces the “trial and error” phase of prescribing, and supports safer medication management.
Our multidisciplinary team, including psychiatrists, nurses, therapists, and support staff, meets daily to review each patient’s progress and adjust treatment plans in real time. Group therapy, individual therapy, medication management, and psychoeducation work together to support healing across multiple dimensions. This integrated approach is essential for patients who are also struggling with substance use disorders, as they may be “self-medicating” to slow down a manic brain, cope with psychotic symptoms, or lift a depressive fog. True Life Care is an out-of-network provider and accepts PPO plans, which allows us to maintain the clinical depth necessary for these complex, dual-diagnosis cases.
By addressing bipolar disorder, depression, psychosis, and schizophrenia-related concerns together, inpatient care can provide a stronger foundation for lasting recovery and safer step-down treatment. We focus on the “whole person” rather than just the diagnosis, ensuring that every aspect of the patient’s mental health is addressed during their stay.

Holistic Integration and Transitioning to Outpatient Care in New Jersey
The “hardest” lesson of all is often the transition. Leaving the 24/7 safety of an inpatient program can be terrifying for both the patient and their family. That is why the transition must be a “step-down,” not a “drop-off.” At True Life Care, we view the inpatient stay as the foundation upon which a larger recovery structure is built. The goal is to move from the controlled environment of the hospital to the real-world environment of the home while maintaining a high level of clinical support.
Lesson 7: Holistic tools sustain the progress made in clinical settings.
Clinical stability is the foundation, but holistic tools are the walls and roof of your recovery. We integrate various modalities to ensure the mind and body heal together, recognizing that physical health and mental health are inextricably linked:
- Yoga and Mindfulness: These practices help regulate the nervous system, reduce cortisol levels, and provide patients with a way to ground themselves during moments of high anxiety or agitation.
- Art and Music Therapy: These offer non-verbal expression for complex emotions that are often difficult to put into words, especially after a traumatic manic or depressive episode. They allow for the processing of feelings that the conscious mind may not yet be ready to articulate.
- Family Therapy: Because bipolar disorder affects the entire household, we involve family members in the healing process. This helps repair relationships damaged during mood episodes and builds a supportive home environment where the patient can continue to thrive.
- Nutritional Psychiatry: Understanding how diet and gut health affect mood regulation is a growing field, and we incorporate these principles to support overall brain health.
Our bipolar disorder treatment in Matawan emphasizes this holistic approach. As an out-of-network provider, we accept PPO plans to ensure you have access to these premium, comprehensive services. We transition patients from acute care into our Partial Hospitalization Program (PHP) or Intensive Outpatient Program (IOP), allowing them to practice their new skills in the real world while still receiving expert psychiatric care and group support several times a week. This continuum of care is vital for preventing the “revolving door” of psychiatric hospitalization.
Navigating Insurance and Access to Care
We know that during a mental health crisis, the last thing you or your family wants to think about is paperwork, insurance codes, and pre-authorizations. However, understanding your coverage is vital for long-term peace of mind and ensuring that the focus remains entirely on recovery. Accessing high-quality psychiatric care should not be an additional source of stress during an already difficult time.
Lesson 8: Quality care is accessible through proper insurance navigation.
True Life Care is an out-of-network provider and accepts PPO plans. This status allows us to provide a higher level of individualized care and a more comprehensive range of services than many in-network facilities. Our dedicated admissions team handles the heavy lifting of insurance verification and pre-authorization so you can focus on the work of healing. We work closely with insurance carriers to advocate for the level of care our patients need.
Lesson 9: Location matters—finding peace in Monmouth County.
There is a reason we chose Matawan, NJ for our facility. Recovery requires an environment that feels different from the one where the crisis occurred. Whether you are coming from Monmouth County or surrounding areas in New Jersey and New York, our facility offers a serene, professional space to reset. Being located in Matawan allows us to help Monmouth County residents access structured inpatient support, group therapy, depression treatment, and psychiatric stabilization close to home while still benefiting from a calm, therapeutic setting. The physical environment is designed to be a sanctuary, promoting reflection and healing away from the triggers of daily life.
Frequently Asked Questions about Inpatient Bipolar Care
What is the typical length of stay for bipolar stabilization?
Most acute inpatient programs for bipolar disorder aim for stabilization within 5 to 12 days. This is the “short-term” phase where the goal is safety and medication adjustment. However, we often recommend a transition to a bipolar disorder treatment center NJ for residential or PHP care, which can last 30 to 45 days for true long-term stability. The brain needs time to adjust to new chemical balances, and rushing this process often leads to rapid relapse. Stabilization is about more than just stopping the crisis; it’s about building a foundation for the future.
Lesson 10: Stabilization is a marathon, not a sprint.
Don’t rush the process. Your brain needs time to adjust to new chemical balances and the psychological impact of the episode. Healing the neurobiology of bipolar disorder takes time, patience, and consistent clinical support.
How does inpatient care address psychiatric emergencies?
We provide 24/7 nursing and immediate access to psychiatrists. In a True Life Care emergency, the focus is on rapid medication adjustment, environmental safety, and clinical stabilization. We remove the stressors of daily life—work, bills, family conflict—so the brain can “cool down” from a manic, depressive, psychotic, or otherwise acute psychiatric state. Our staff is trained in de-escalation techniques that prioritize the patient’s dignity while ensuring safety for everyone in the facility.
How important is group therapy in inpatient bipolar treatment?
Group therapy is a central part of effective inpatient care. It helps patients reduce isolation, learn practical coping skills, receive peer support, and practice healthier communication. Group therapy can also be especially valuable for individuals recovering from bipolar depression, psychosis, or relationship damage caused by a mood episode. In many cases, healing becomes more sustainable when patients feel understood by others who have lived through similar experiences. It provides a sense of belonging that is often lost during a mood episode.
Does inpatient treatment help with bipolar depression?
Yes. Depression treatment is a core component of inpatient bipolar care. Patients may receive psychiatric evaluation, medication adjustment, CBT, DBT, psychoeducation, and structured support for suicidal thoughts, hopelessness, fatigue, or severe withdrawal. Because bipolar depression can be complex and may not respond to traditional antidepressants alone, treatment focuses on improving safety while building a long-term plan for mood stability using mood stabilizers and other specialized medications.
Can inpatient programs treat schizophrenia-related symptoms too?
In many cases, yes. Bipolar disorder can overlap with psychosis or schizophrenia-spectrum presentations, and careful psychiatric assessment is essential. Our clinical team evaluates whether symptoms point to bipolar disorder with psychotic features, schizoaffective disorder, or another condition requiring specialized care. Treatment may include medication management, close observation, individual therapy, and supportive group therapy tailored to those experiencing reality distortion.
Can family members participate in the treatment process?
Absolutely. In fact, it’s highly recommended. We offer family forums and education sessions because bipolar disorder is often misunderstood by loved ones as “bad behavior” or “laziness.” Education helps families become a part of the support system rather than a source of stress. You can find more about finding bipolar therapy in NJ that involves the whole family in the recovery journey.
What happens if I have a co-occurring substance use disorder?
Many individuals with bipolar disorder use substances to cope with their symptoms. Our program is dual-diagnosis capable, meaning we treat both the mood disorder and the addiction simultaneously. Treating one without the other is rarely successful in the long term, as the two conditions often feed into each other in a destructive cycle.
Do you help people in Monmouth County?
Yes. From our Matawan, NJ location, we help Monmouth County residents and surrounding communities access inpatient mental health support, crisis stabilization, group therapy, depression treatment, and step-down planning for continued healing. We are proud to be a resource for our local community.
What insurance do you accept?
True Life Care is an out-of-network provider and accepts PPO plans. Our admissions team can help verify benefits and guide families through the next steps of the insurance process.
Is the facility private?
Yes, True Life Care provides a private, professional environment. As an out-of-network provider accepting PPO plans, we maintain a high standard of privacy and individualized attention for every patient, ensuring a discreet and respectful healing environment.
Conclusion
Bipolar disorder is a formidable opponent, but it is not unbeatable. The lessons learned in inpatient programs for bipolar disorder are often hard-won, but they provide the “owner’s manual” for your own brain. By combining expert psychiatric care, evidence-based group therapy, and a structured environment, we help our patients move from the chaos of mood swings to the steady ground of recovery. The journey to stability requires courage, but you do not have to walk it alone.
At True Life Care, we are committed to providing personalized, evidence-based healing. From our Matawan, NJ location, we serve residents across Monmouth County and the surrounding NJ/NY areas with a focus on long-term recovery. We don’t just want to stop the current crisis; we want to help you build a life where the next one never happens. Our approach integrates the best of clinical science with compassionate, holistic care to ensure that every patient has the tools they need for a sustainable future. True Life Care is an out-of-network provider and accepts PPO plans, offering the specialized attention required for complex mood disorders.
If you are ready to reclaim your life and find the stability you deserve, we are here to help. True Life Care offers the expert psychiatric care and supportive community you need to begin your healing process. Start your journey to stability today.